Illiac Vein Stenting
After many years of success and improvements in angioplasty and stenting to treat the arteries that supply the heart, legs and kidneys with blood, it is becoming more common to use these procedures to treat other conditions, such as DVT and pelvic congestion.
Alpharetta Illiac Vein Stenting
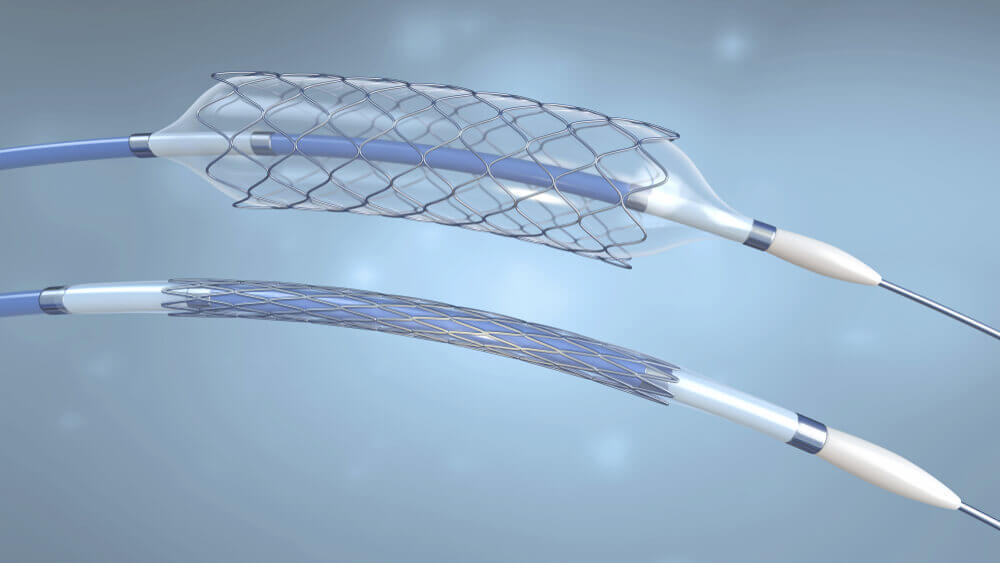
The two main mechanisms for venous diseases are reflux and obstruction, with some patients having a combination of the two. A potential cause of venous insufficiency is obstruction and/or compression of large veins in the pelvis. Guided by the use of intravascular ultrasound (IVUS), this condition can now be treated successfully with stent insertion. IVUS is thus the new gold standard in detecting iliac and caval venous obstructive lesions.
In the past, treatment for deep venous disease involved open surgery for venous bypass. With the development of endovascular techniques, venous angioplasty and stenting are now better treatment options for patients suffering from obstructive venous disease. Heart and Vascular Care has been recognized for offering high-quality outpatient vein treatment by the Accreditation Association for Ambulatory Health Care (AAAHC).
How Does It Work?
IVUS uses sound waves to produce an image of the diseased vein and to see their condition. The sound waves travel through a tube called a catheter. Through a tiny incision, a catheter that has a small ultrasound device mounted on it, is inserted into the iliac vein or artery. Then, this ultrasound device uses sound waves to map the inside of the veins and arteries, allowing our vascular surgeons to identify any vein compression.
What does the procedure look like?
Using image guidance, the tip of a catheter is inserted through the skin into a vein and advanced across the site of a suspected venous blockage. In this process, a stent may be placed at the treatment site to hold the vein open.
Are there any side effects?
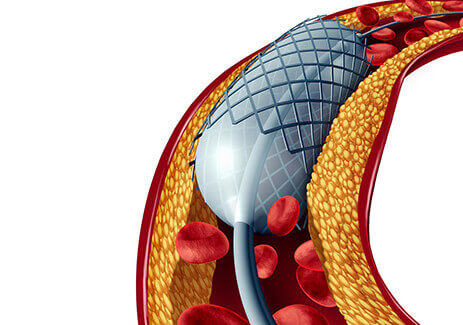
The side effects of stent placement are few and usually minor. They can include bruising at the point where the catheter enters the vein. This bruising is usually harmless and should spontaneously heal. Cold or warm packs as preferred may be applied to the area if bruising is extensive.
How should you prepare for treatment?
You should report to your doctor all medications that you are taking, including herbal supplements, and if you have any allergies, especially to local anesthetic medications, general anesthesia or contrast materials sometimes referred to as dye. Your physician may advise you to stop taking aspirin, nonsteroidal anti-inflammatory drugs (NSAIDs), or blood thinners for a specified period of time before your procedure. Also, inform your doctor about recent illnesses or other medical conditions.
